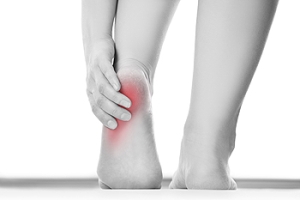
Why Pain in Your Heel May Be Worse in the Morning
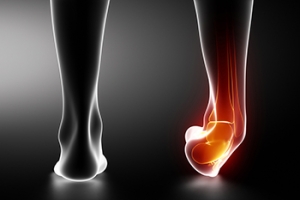
There are different conditions that cause stiffness or pain in your heel that gets worse in the morning. Pain from conditions such as plantar fasciitis—where the long band of tissue on the bottom of the foot becomes inflamed—can be worse in the morning because blood supply to the feet is reduced while you sleep. Similarly, an inflammation of the tissue that connects the heel bone with the calf muscles (Achilles tendinitis) can also be more painful upon waking. This can also be caused by poor circulation, or the fact that calf muscles are shortened while at rest and may become painful when they are stretched as you take your first steps. Unlike plantar fasciitis, however, heel pain from Achilles tendinitis typically does not subside after moving around and warming up the heel. If you have any pain in your heel, seek the care of a podiatrist to determine its cause and the best course of treatment.
Many people suffer from bouts of heel pain. For more information, contact John Mccain, DPM of Advanced Foot & Ankle Specialists, PA. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions, please feel free to contact one of our offices located in Stuart and Jupiter, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Heel Pain
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
Listen to What Your Feet May Be Telling You
Sore feet may sometimes be indicative of an underlying health issue and should not be ignored. If the muscles in your feet cannot relax properly and therefore cramp, this may be an indicator of dehydration, nerve or circulation issues, or possibly even neurological conditions. A foot sore that does not heal can sometimes signal the presence of diabetes. If your feet and toes are always cold, you may have hypothyroidism (an underactive thyroid), or poor circulation which may be the result of any number of health conditions like diabetes, high blood pressure, cardiovascular disease, and more. Arthritis often presents itself first in small joints such as those in the toes. If you notice any soreness or pain in your feet, an examination by a podiatrist is the first step in helping to determine the underlying cause.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with John Mccain, DPM from Advanced Foot & Ankle Specialists, PA. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact one of our offices located in Stuart and Jupiter, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
The feet, being the foundation of the body, carry all of the body’s weight and are therefore prone to experiencing pain and discomfort. If you are experiencing foot pain, it is important to determine where in the foot you are experiencing this pain to help discover the cause of it. While pain can be experienced virtually anywhere in the foot, the most common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles tendinitis, and heel spurs. Pain experienced in the ankle can be a sign of an ankle sprain, arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious cases, pain in the foot can be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and warmth in the affected area. Whether the pain can be described as sharp or dull depends on the foot condition behind it. It is important to visit your local podiatrist if your foot pain and its accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe certain treatments. These treatments can include but are not limited to prescription or over-the-counter drugs and medications, certain therapies, cortisone injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and ankle specialist to determine the cause and location. He or she will then prescribe the best treatment for you. While milder cases of foot pain may respond well to rest and at-home treatments, more serious cases may take some time to fully recover.
Treating a Broken Toe
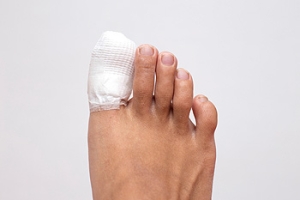
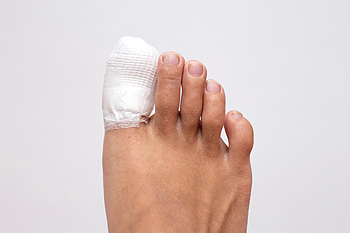 People who have endured a broken toe may understand how it can hinder accomplishing daily activities. It can happen as a result from dropping a heavy object on it, or by jamming it into a piece of furniture. The small bones that exist in toes can be more susceptible to becoming broken and this is especially true for the pinky toe. Common symptoms that many patients experience during a broken toe can consist of bruising, swelling, and it is often difficult to walk. After a proper diagnosis is performed, which generally involves having an X-ray taken, the proper healing methods can begin. If the fracture is mild, buddy taping may be an effective form of treatment. This is done by taping the broken toe to the toe next to it, which can be successful in providing the necessary support to improve the affected toes stability. If you have broken your toe, it is suggested that you seek the counsel of a podiatrist who can determine what the best course of treatment is for you.
People who have endured a broken toe may understand how it can hinder accomplishing daily activities. It can happen as a result from dropping a heavy object on it, or by jamming it into a piece of furniture. The small bones that exist in toes can be more susceptible to becoming broken and this is especially true for the pinky toe. Common symptoms that many patients experience during a broken toe can consist of bruising, swelling, and it is often difficult to walk. After a proper diagnosis is performed, which generally involves having an X-ray taken, the proper healing methods can begin. If the fracture is mild, buddy taping may be an effective form of treatment. This is done by taping the broken toe to the toe next to it, which can be successful in providing the necessary support to improve the affected toes stability. If you have broken your toe, it is suggested that you seek the counsel of a podiatrist who can determine what the best course of treatment is for you.
A broken toe can be very painful and lead to complications if not properly fixed. If you have any concerns about your feet, contact John Mccain, DPM from Advanced Foot & Ankle Specialists, PA. Our doctor will treat your foot and ankle needs.
What to Know About a Broken Toe
Although most people try to avoid foot trauma such as banging, stubbing, or dropping heavy objects on their feet, the unfortunate fact is that it is a common occurrence. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break (fracture).
Symptoms of a Broken Toe
- Throbbing pain
- Swelling
- Bruising on the skin and toenail
- The inability to move the toe
- Toe appears crooked or disfigured
- Tingling or numbness in the toe
Generally, it is best to stay off of the injured toe with the affected foot elevated.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery. Due to its position and the pressure it endures with daily activity, future complications can occur if the big toe is not properly treated.
If you have any questions, please feel free to contact one of our offices located in Stuart and Jupiter, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What to Know About a Broken Toe
The forefoot is composed of five metatarsal bones and fourteen phalanges. Each toe has three phalanges except for the big toe which only has two. Our toes play an essential role to the walking process, which is why a broken toe could seriously disrupt one’s ability to move around. Toe fractures are common and can be very painful. Fortunately, these injuries rarely require surgery and usually heal with rest and a change in activity.
Broken toes typically result from a traumatic event such as falling, stubbing the toe, or dropping something on the toe. Traumatic toe fractures may be categorized as either minor or severe fractures. At times, one may hear a “pop” or “crack” sound when the bone breaks. Common symptoms of a traumatic toe fracture include pain, throbbing, bruising, swelling, and redness.
Another type of toe fractures is a stress fracture. These injuries usually appear in the form of small hairline breaks on the bone. Stress fractures develop after repetitive activity instead of a single injury. Stress fractures occur when the muscles in the bone become too weak to absorb impact. Consequently, the toe bone becomes vulnerable to any pressure and impact it endures. Symptoms for a stress fracture in the toe include swelling without bruising, tenderness to the touch, pain that goes away with rest, and pain after walking or running.
If you suspect that you have a broken toe, you should make an appointment with your podiatrist. He or she will likely diagnose you by performing a physical exam and an X-ray. Treatment for a broken toe may include the R.I.C.E. method, buddy taping, surgery, or antibiotics. The R.I.C.E. method (Rest, Ice, Compression, and Elevation) is a common treatment method for many injuries because it decreases pain. Buddy tapping involves wrapping the injured toe next to an adjacent toe to keep it supported and protected. These two methods have proven to be effective in the healing process for toe fractures. The estimated healing time for a broken toe is approximately four to six weeks. If the injury becomes infected or requires surgery, the estimated healing time may take eight weeks or more.
The Different Types of Toenail Fungus
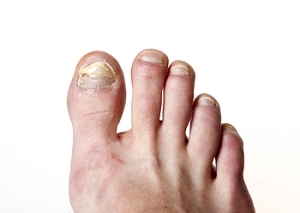
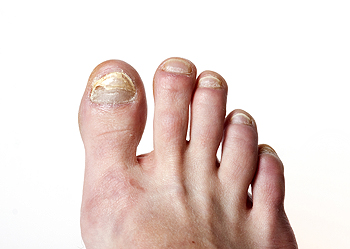
A fungal infection of the toenails is a common condition that affects as much as 10% of the population. There are various types of toenail fungus, better known among medical professionals as onychomycosis. The most common type is distal or lateral subungual onychomycosis. It frequently affects the big toenails and causes yellow, white, or brown discoloration that starts at the end or side of a toenail before spreading to the rest of the nail. Proximal subungual onychomycosis starts at the base of the toenail and spreads outwards. Superficial onychomycosis first infects the top layers of the toenails and then spreads to deeper layers. Regardless of the type of toenail fungus you may have, treatment methods such as oral and topical antifungal medications or laser therapy can help. To learn more about toenail fungus and available treatment options, schedule an appointment with a podiatrist near you.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact John Mccain, DPM of Advanced Foot & Ankle Specialists, PA. Our doctor can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions please contact one of our offices located in Stuart and Jupiter, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Treating Toenail Fungus
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
How Did I Sprain My Ankle?
 Sprained ankles are one of the most common injuries among athletes. Sprains occur when the ligaments that connect to the bones become inflamed or torn. Ankle sprains are usually noticeable right away, and they are often a result of the foot turning inwards under the body’s weight. Pain can also be felt throughout the ankle, and the joint will likely swell and become bruised. Common treatment methods for sprained ankles include ice, rest, an ankle brace, and ankle taping. However, it can be difficult to tell the difference between an ankle sprain and a fractured or broken ankle. Because of this, patients who believe that they have sprained their ankle should consult with a podiatrist for a proper diagnosis and advised treatment plan.
Sprained ankles are one of the most common injuries among athletes. Sprains occur when the ligaments that connect to the bones become inflamed or torn. Ankle sprains are usually noticeable right away, and they are often a result of the foot turning inwards under the body’s weight. Pain can also be felt throughout the ankle, and the joint will likely swell and become bruised. Common treatment methods for sprained ankles include ice, rest, an ankle brace, and ankle taping. However, it can be difficult to tell the difference between an ankle sprain and a fractured or broken ankle. Because of this, patients who believe that they have sprained their ankle should consult with a podiatrist for a proper diagnosis and advised treatment plan.
Ankle sprains are common but need immediate attention. If you need your feet checked, contact John Mccain, DPM from Advanced Foot & Ankle Specialists, PA. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains take place when the ligaments in your ankle are torn or stretched beyond their limits. There are multiple ways that the ankle can become injured, including twisting or rolling over onto your ankle, putting undue stress on it, or causing trauma to the ankle itself.
What Are the Symptoms?
- Mild to moderate bruising
- Limited mobility
- Swelling
- Discoloration of the skin (depending on severity)
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
Treatment of a sprain depends on the severity. Many times, people are told to rest and remain off their feet completely, while others are given an air cast. If the sprain is very severe, surgery may be required.
If you have suffered an ankle sprain previously, you may want to consider additional support such as a brace and regular exercises to strengthen the ankle.
If you have any questions please feel free to contact one of our offices located in Stuart and Jupiter, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.